Family members of patients recently discharged from the hospital may have a higher risk of getting an antibiotic-resistant infection, often called a superbug, even if the patient was not diagnosed with the same infection, suggesting hospitals play a role in the community spread of resistant bacteria, according to study in Infection Control & Hospital Epidemiology, the journal of the Society for Healthcare Epidemiology of America.
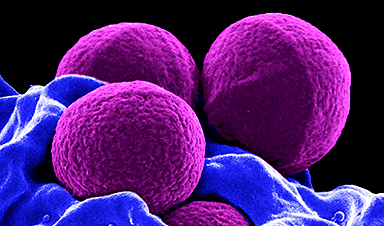
When recently hospitalized patients were diagnosed with the superbug -; Methicillin-resistant Staphylococcus aureus infection (MRSA) -; the risk to relatives living with them was even higher. The longer the relative’s hospital stay, even without a MRSA diagnosis, the higher the risk to family members.
Patients can become colonized with MRSA during their hospital stay and transmit MRSA to their household members. This suggests hospitals contribute to the spread of MRSA into the community through discharged patients who are asymptomatic carriers.”
Aaron Miller, PhD, lead researcher on the study and research assistant professor of internal medicine-infectious diseases, University of Iowa
Miller recommends hospitals enhance infection control practices, including testing for MRSA colonization, especially at discharge, even with there are no symptoms of infection. He said MRSA colonization and infections could be tracked among hospital patients and their household contacts to identify and mitigate transmission more effectively.
“This important study illustrates the risk of spread of resistant pathogens related to healthcare and highlights the essential importance of core infection practices,” said SHEA President Thomas Talbot, M.D., chief hospital epidemiologist at Vanderbilt University Medical center. Talbot was not involved with the research. “Hand hygiene, environmental cleaning, and standard interventions to reduce Staphylococcal colonization are crucial to preventing the spread of resistant bacteria in healthcare settings,”
MRSA infections are known as superbugs because they do not respond to common antibiotics, making them difficult to treat. MRSA generally occurs in people who have been in a hospital or another health care setting, such as a nursing home, but MRSA also spreads in communities outside the hospital, usually through skin-to-skin contact. Most people with MRSA have no symptoms, but the bacteria can cause painful swelling if it gets under the skin, and it can be deadly if it spreads to other parts of the body, such as blood or lungs.
Researchers used a large database of insurance claims that included 158 million enrollees with two or more family members on the same plan to learn about how MRSA spread to after someone in a household had been in the hospital.
Reviewing 424,512 MRSA cases among 343,524 insured people, the study found 4,724 cases of MRSA being potentially transmitted to a family member from a relative who had recently been in the hospital and had a diagnosis of MRSA. They also found 8,064 potential transmissions of MRSA after the hospitalization of a family member who did not have a MRSA infection.
“It is important not over-emphasize the hospital stay risk,” Miller said. “While we identified a significant risk factor for transmission in the household and community the absolute risk remains relatively low.”
People exposed to a recently hospitalized family member with MRSA were more than 71 times, or 7000%, more likely to get a MRSA infection compared to enrollees who did not have a family member who had been in the hospitalized or exposed to MRSA in the previous 30 days.
Having a family member in the household who was hospitalized but did not have MRSA increased the chances of a relative getting MRSA in the month after discharge by 44%.
The more time the family member spent in the hospital, the higher the likelihood someone in their household would get MRSA. If the patient was in the hospital one to three days in the previous month, the chance of a relative getting MRSA increased by 34% compared to people with no recent hospitalizations in their household. If a family member was hospitalized for four to 10 days, the chances of MRSA infection in a relative were 49% higher, and with hospitalizations longer than 10 days the odds of relative in the same household getting an infection rose by 70% to 80%.
Other factors associated with MRSA infections among household members included number of other illnesses, prior antibiotic usage, and the presence of young children in the family.
The study, “Hospitalizations among family members increase the risk of MRSA infection in a household,” was published online in Infection Control & Hospital Epidemiology on August 7.
Miller A. C., et al. (2024). Hospitalizations among family members increase the risk of MRSA infection in a household. Infection Control & Hospital Epidemiology. doi.org/10.1017/ice.2024.106.
News
Turning Off Nerve Signals: Scientists Develop Promising New Pancreatic Cancer Treatment
Pancreatic cancer reprograms nerve cells to fuel its growth, but blocking these connections can shrink tumors and boost treatment effectiveness. Pancreatic cancer is closely linked to the nervous system, according to researchers from the [...]
New human antibody shows promise for Ebola virus treatment
New research led by scientists at La Jolla Institute for Immunology (LJI) reveals the workings of a human antibody called mAb 3A6, which may prove to be an important component for Ebola virus therapeutics. [...]
Early Alzheimer’s Detection Test – Years Before Symptoms Appear
A new biomarker test can detect early-stage tau protein clumping up to a decade before it appears on brain scans, improving early Alzheimer’s diagnosis. Unlike amyloid-beta, tau neurofibrillary tangles are directly linked to cognitive decline. Years [...]
New mpox variant can spread rapidly across borders
International researchers, including from DTU National Food Institute, warn that the ongoing mpox outbreak in the Democratic Republic of the Congo (DRC) has the potential to spread across borders more rapidly. The mpox virus [...]
How far would you trust AI to make important decisions?
From tailored Netflix recommendations to personalized Facebook feeds, artificial intelligence (AI) adeptly serves content that matches our preferences and past behaviors. But while a restaurant tip or two is handy, how comfortable would you [...]
Can AI Really Think? Research Reveals Gaps in Logical Execution
While AI models can break down problems into structured steps, new research reveals they still fail at basic arithmetic and fact-checking—raising questions about their true reasoning abilities. Large Language Models (LLMs) have become indispensable [...]
Scientists Just Made Cancer Radiation Therapy Smarter, Safer, and More Precise
Scientists at UC San Francisco have developed a revolutionary cancer treatment that precisely targets tumors with radiation while sparing healthy tissues. By using a KRAS-targeting drug to mark cancer cells and attaching a radioactive [...]
Superbugs Are Losing to Science, Light, and a Little Spice
Texas A&M researchers have found that curcumin, when activated by light, can weaken antibiotic-resistant bacteria, restoring the effectiveness of conventional antibiotics. Curcumin: A Surprising Ally Against Superbugs In 2017, a woman admitted to a [...]
New Research Shatters the Perfect Pitch Myth
For decades, people believed absolute pitch was an exclusive ability granted only to those with the right genetics or early music training. But new research from the University of Surrey proves otherwise. It’s been [...]
Why Some Drinkers Suffer Devastating Liver Damage While Others Don’t
A study from Keck Medicine of USC found that heavy drinkers with diabetes, high blood pressure, or a large waistline are up to 2.4 times more likely to develop advanced liver disease. These conditions may amplify [...]
“Good” Cholesterol Could Be Bad for Your Eyes – New Study Raises Concerns
‘Good’ cholesterol may be linked to an increased risk of glaucoma in individuals over 55, while, paradoxically, ‘bad’ cholesterol may be associated with a lower risk. These findings challenge conventional beliefs about factors that [...]
Reawakening Dormant Nerve Cells: Groundbreaking Neurotechnology Restores Motor Function
A new electrical stimulation therapy for spinal muscle atrophy (SMA) has shown promise in reactivating motor neurons and improving movement. In a pilot clinical trial, three patients who received spinal cord stimulation for one [...]
AI’s Energy Crisis Solved? A Revolutionary Magnetic Chip Could Change Everything
AI is evolving at an incredible pace, but its growing energy demands pose a major challenge. Enter spintronic devices—new technology that mimics the brain’s efficiency by integrating memory and processing. Scientists in Japan have [...]
Nanotechnology for oil spill response and cleanup in coastal regions
(Nanowerk News) Cleaning up after a major oil spill is a long, expensive process, and the damage to a coastal region’s ecosystem can be significant. This is especially true for the world’s Arctic region, [...]
The Role of Nanotechnology in Space Exploration
Nanotechnology, which involves working with materials at the atomic or molecular level, is becoming increasingly important in space exploration. By improving strength, thermal stability, electrical conductivity, and radiation resistance, nanotechnology is helping create lighter, more [...]
New Study Challenges Beliefs About CBD in Pregnancy, Reveals Unexpected Risks
CBD is gaining popularity as a remedy for pregnancy symptoms like nausea and anxiety, but new research suggests it may not be as safe as many believe. A study from McMaster University found that [...]