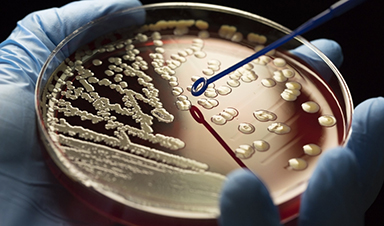
Increasing drug resistance could leave us powerless to fight infections we now consider routine, and scientists are urgently searching for answers.
It was just a urinary tract infection (UTI). Helen Osment, a fundraiser from Hertfordshire, had had them before and she knew the symptoms. When she called the doctor with pain, a burning sensation and blood in her urine, they prescribed a course of antibiotics – a few days of nitrofurantoin.
But this time, her UTI didn’t go away. It got worse. The pain was bad and she started feeling feverish. As her symptoms failed to improve, she felt uncomfortable and miserable. “I think it can affect you mentally when you have one, it can make you feel quite sort of down and low,” she says.
Her doctor tried another antibiotic, trimethoprim, but the infection remained. Still feeling awful, she asked the doctor for “something stronger”. Options were limited by the fact that Osment had been deemed allergic to penicillin as a child, and this was flagged on her records (though like many who are flagged as allergic, she later turned out not to be). She was prescribed ciprofloxacin but reacted badly: she felt heart palpitations and pain in her knee, which turned out to be tendonitis, a potential side-effect of the drug. She visited a walk-in centre, where she was told to stop taking it and was put on a longer course of nitrofurantoin.
Her condition deteriorated. Feverish and in so much pain she couldn’t even pick up her baby, she ended up in A&E. “I was thinking, oh surely they’ll just give me some more antibiotics,” she says. “I didn’t realise how ill I was.” The mastitis had formed a large abscess and Osment had developed sepsis – a life-threatening condition caused by the body’s response to an infection. Luckily, this was caught early, and after being hospitalised and put on a different antibiotic intravenously, she beat the infection and recovered.
“It just goes to show that it can happen to anybody, and things can escalate very quickly,” Osment says. She now shares her story through the charity Antibiotic Research UK, to help raise awareness of antimicrobial resistance.
When Covid-19 began to spread around the globe, it was something we hadn’t seen before and we had no medicines to defend ourselves against it. But it’s not only new pathogens, like Sars-CoV-2, that pose a threat to global human health. Antimicrobial resistance means that existing bugs – ones we perhaps don’t worry too much about – are becoming resistant to the treatments we have come to take for granted, such as antibiotics. As this resistance becomes more common, we could find ourselves in a similar situation: facing infectious diseases with limited treatment options.
Our experience under Covid-19 may have given us a glimpse of that future. “It shows what the world would be like if we had resistance to all known antibiotics,” says Jessica Boname, former head of antimicrobial resistance at the UK’s Medical Research Council. “We would be in the Covid-19 world.”
The term antibiotic resistance refers specifically to bacteria becoming resistant to antibiotics. Antimicrobial resistance is a broader term that also covers other microbes such as fungi, parasites and viruses.
Today, if we get an infection, we generally expect that we can go to the doctor and get some medicine to treat it. But if the microbes causing the infection are resistant to that medicine, the infection may not go away. We might go on to try another drug, and another, and another, but if the microbes are resistant to those too, we’re back at square one. Microbes that are able to resist multiple antimicrobials are sometimes referred to as “superbugs” – and they can be very difficult to treat.
The stakes are high. If antimicrobial resistance is left to rise unchecked, we may no longer be able to knock out common infections with a simple prescription. Illnesses caused by resistant pathogens will require longer, more costly treatment. In more and more cases, we may not be able to treat a resistant infection at all.
And it’s not just routine infections that will become more dangerous as we lose more antimicrobials from our medical arsenal. Much of modern medicine is built on the assumption that we can easily fight or prevent infection. If this is no longer the case, these foundations start to crumble.
Take surgery: antibiotics are given as a preventative measure before and after many operations that have a high risk of infection, such as hip replacements, organ transplants or Caesarean sections. If we can no longer count on antimicrobials being effective, surgery will become much more risky. In some cases, it may be unviable: the risk of getting an untreatable infection will simply be too high.
For most infections, we have multiple lines of defence. If one antimicrobial doesn’t work, you try another, then another, and so on until you reach those that are held back as a last resort, to be used only in extremely limited cases so as to prevent resistance from occurring. As these antimicrobials are struck down by resistance, the obvious solution would be to make new ones. But we aren’t developing them fast enough.
According to the World Health Organisation, lack of innovation and funding is a major concern, with most new products in development showing little extra benefit and few targeting some of the most urgent infections.
Most of the antimicrobial substances that we commonly use today were found in the 40s and 50s, soon after penicillin – a “golden era” for antibiotic discovery. But in the following decades, discoveries of new antibiotics were few and far between. The low-hanging fruit had been found and scientists were getting frustrated at discovering the same compounds again and again.
In the latter part of the 20th century, a new method was adopted. Rather than screening natural compounds to search for antimicrobial substances, scientists decided to try a more targeted approach. They set out to look specifically for compounds that inhibited pathways essential to the function of bacteria. If you know a bacterium needs to create a certain enzyme to thrive, for instance, then finding a compound that inhibits the production of this enzyme could give you a promising lead for a new antimicrobial drug. Researchers turned their attention to synthetic compounds in the vast chemical libraries of research groups and pharmaceutical companies.
It’s an approach that has been successful for discovering many kinds of drugs, but it didn’t really work for antimicrobials. “They were new technologies at the time, we thought they were going to generate lots of really useful compounds,” says Mathew Upton, a professor of medical microbiology at the University of Plymouth. “And they basically generated nothing at all.”
It’s not that we didn’t find anything – promising compounds were identified – but when tested they just didn’t work in actual bacteria. And so the focus turned once again to natural substances, making the most of the tiny, living antibiotic factories in the environment all around us. These days, the way many researchers find new antibiotics is not all that dissimilar to Alexander Fleming’s observation of mould on a sample dish, albeit rather more deliberate.
The reason for searching in places so far removed from our everyday environment is that it increases the chance of finding a truly novel antibiotic compound, Upton explains. Often, researchers can find a substance with promising antibiotic properties, but once they’ve gone through the hassle of growing the microbe in the lab and purifying the compound, they find out it is the same as, or similar to, an existing antibiotic – and will therefore likely be disarmed by the same resistance mechanisms.
“If a compound is the same as something we’ve seen before, or very related to it, it’s probably not going to be worth developing, because any resistance mechanism that is already out there will undermine it as soon as we use it in the clinic,” Upton says.
But we don’t always need to look so far away from home. Upton is currently working with one compound that was found in a sample taken from the surface of human skin.
But ultimately, the things that could have the most impact are the ones we already know about – like access to clean water and sanitation, infection prevention and control measures, and improved access to existing vaccines and treatments. Similarly, if we can improve infection control measures in hospitals, we will reduce the spread of hospital-acquired infections. When people do get infections, we need to be better at treating them – using the right antimicrobials in the right patients, at the right doses. We also need to reconsider our use of antimicrobials in agriculture and the environment.
Individuals can refrain from asking for antibiotics when they have a cold and follow the instructions when they are prescribed them. Prescribers can make sure they’re sticking to stewardship guidelines.
A multitude of solutions are needed to address many different issues. Just as we have seen with the Covid-19 pandemic, we need researchers, clinicians, engineers, politicians, behavioural scientists and economists to work together across borders.
News
RNA Recycling Extends Lifespan
Summary: Researchers discovered a biological “trash disposal” mechanism that directly controls how fast we age. While circular RNA has long been known to accumulate in cells as we get older, this study proves for the [...]
Cancer’s Deadly Paradox: How Tumors Break Their Own DNA To Keep Growing
Cancer’s strongest gene switches push DNA into damaging overdrive, creating repeated breaks and repairs that may fuel tumor evolution while exposing possible therapeutic weak spots. A new study indicates that cancer can harm its own genetic [...]
NanoMedical Brain/Cloud Interface – Explorations and Implications. A new book from Frank Boehm
New book from Frank Boehm, NanoappsMedical Inc Founder: This book explores the future hypothetical possibility that the cerebral cortex of the human brain might be seamlessly, safely, and securely connected with the Cloud via [...]
Our books now available worldwide!
Online Sellers other than Amazon, Routledge, and IOPP Indigo Global Health Care Equivalency in the Age of Nanotechnology, Nanomedicine and Artifcial Intelligence Global Health Care Equivalency In The Age Of Nanotechnology, Nanomedicine And Artificial [...]
Ryugu asteroid samples contain all DNA and RNA building blocks, bolstering origin-of-life theories
All the essential ingredients to make the DNA and RNA underpinning life on Earth have been discovered in samples collected from the asteroid Ryugu, scientists said Monday. The discovery comes after these building blocks [...]
Is Berberine Really a “Natural Ozempic”?
Often labeled a “natural Ozempic,” berberine is widely discussed as a metabolic aid. Yet research suggests its influence may lie deeper. In recent years, berberine has gained significant attention as a supposed “natural way” [...]
Viagra Ingredient Shows Promise for Rare Childhood Brain Disease in Surprising Study
A rare childhood disease with no approved treatment may have an unexpected new therapeutic candidate. Sildenafil, the active ingredient also sold under the brand name Viagra, may help reduce symptoms in people with Leigh [...]
In a first for China, Neuracle’s implantable brain-computer interface wins approval
In a landmark development, Neuracle Medical Technology has secured the country’s first-ever approval for an implantable brain-computer interface (BCI) system designed to restore hand motor function in patients with spinal cord injuries, in a [...]
A Cambridge Lab Mistake Reveals a Powerful New Way to Modify Drug Molecules
A surprising lab discovery reveals a light-powered way to tweak complex drugs faster, cleaner, and later in development. Researchers at the University of Cambridge have created a new technique for altering complex drug molecules [...]
New book from NanoappsMedical Inc – Molecular Manufacturing: The Future of Nanomedicine
This book explores the revolutionary potential of atomically precise manufacturing technologies to transform global healthcare, as well as practically every other sector across society. This forward-thinking volume examines how envisaged Factory@Home systems might enable the cost-effective [...]
Scientists Discover Simple Saliva Test That Reveals Hidden Diabetes Risk
Researchers have identified a potential new way to assess metabolic health using saliva instead of blood. High insulin levels in the blood, known as hyperinsulinemia, can reveal metabolic problems long before obvious symptoms appear. It is [...]
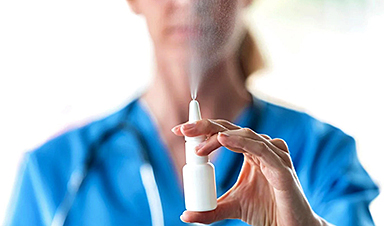
One Nasal Spray Could Protect Against COVID, Flu, Pneumonia, and More
A single nasal spray vaccine may one day protect against viruses, pneumonia, and even allergies. For decades, scientists have dreamed of creating a universal vaccine capable of protecting against many different pathogens. The idea [...]
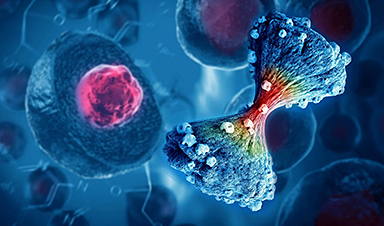
New AI Model Predicts Cancer Spread With Incredible Accuracy
Scientists have developed an AI system that analyzes complex gene-expression signatures to estimate the likelihood that a tumor will spread. Why do some tumors spread throughout the body while others remain confined to their [...]
Scientists Discover DNA “Flips” That Supercharge Evolution
In Lake Malawi, hundreds of species of cichlid fish have evolved with astonishing speed, offering scientists a rare opportunity to study how biodiversity arises. Researchers have identified segments of “flipped” DNA that may allow fish to adapt rapidly [...]
Scientists Discover Why Some COVID Survivors Still Can’t Taste Food Years Later
A new study provides the first direct biological evidence explaining why some people continue to experience taste loss long after recovering from COVID-19. Researchers have uncovered specific biological changes in taste buds that could help [...]
Catching COVID significantly raises the risk of developing kidney disease, researchers find
Catching Covid significantly raises the risk of developing deadly kidney disease, research has shown. The virus was found to increase the chances that patients will develop the incurable condition by around 50 per cent. [...]